Lorrca for Pharma
Sickle Cell Disease
More than 20 million individuals are living with sickle cell disease (SCD) world-wide. Sickle cell disease, a rare, genetically inherited condition, which affects haemoglobin, the protein in red blood cells that carries oxygen throughout the body.
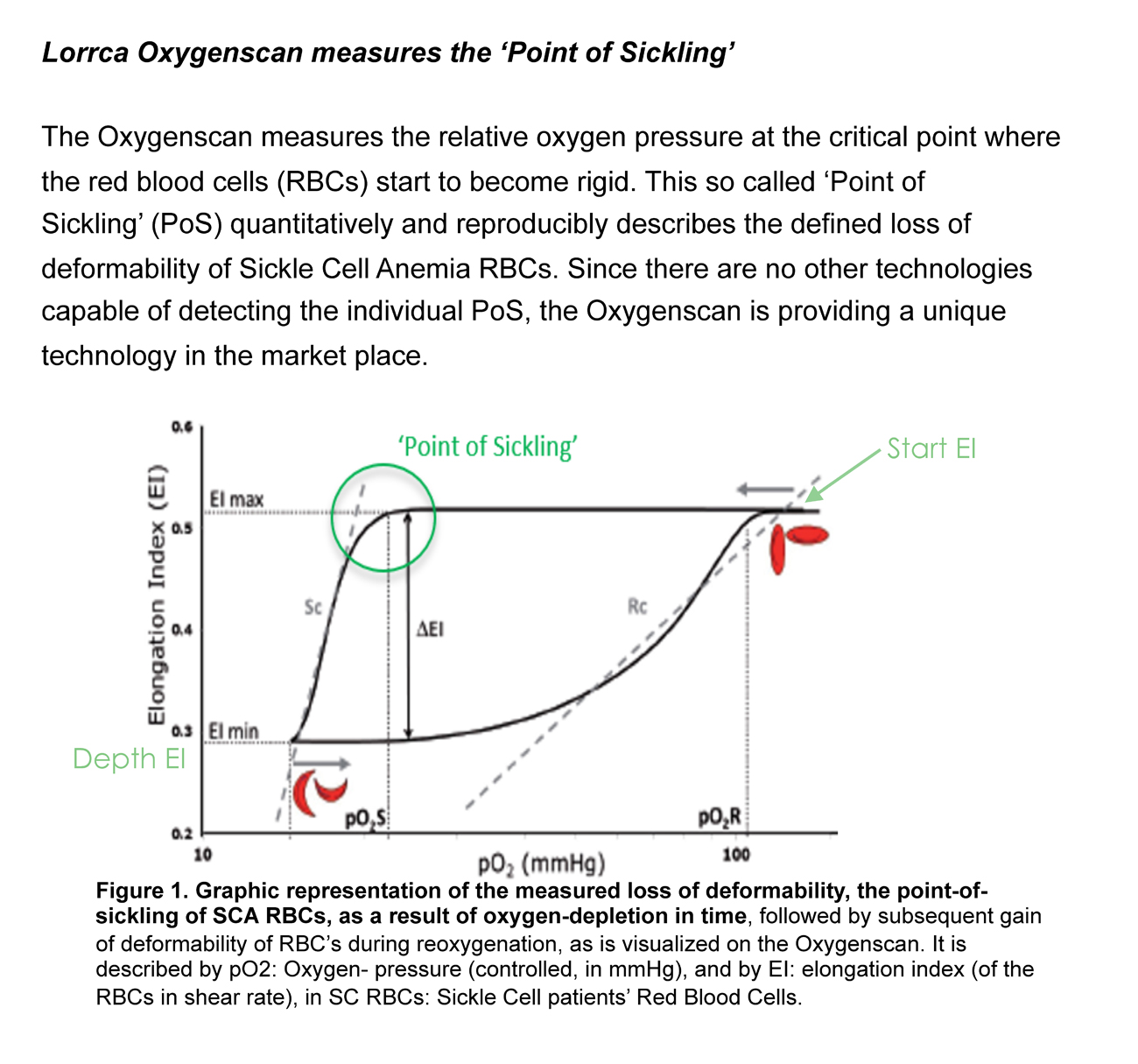
Healthy RBC are small and flexible, and they have the ability to flow throughout capillaries, the smallest veins in the body. In patients with sickle cell disease, RBC that express the mutant, the sickle form, of haemoglobin (HbSS) polymerizes to form fibers that make RBC less flexible and sickled under low oxygen conditions in the peripheral capillaries.
These sickled blood cells are stiff and angular, and they may get stuck on one another or other cells in the blood leading to occlusion or blockage of vessels in micro capillary beds. Sickled blood cells also become damaged as they collide with the blood vessel walls, further activating immune cells and making them and the vessel wall “stickier”.
Sickle cell disease damages many organs in patients including the lungs, kidneys, brain, liver, spleen and results in daily pain for patients and progressively, frequent hospitalizations.